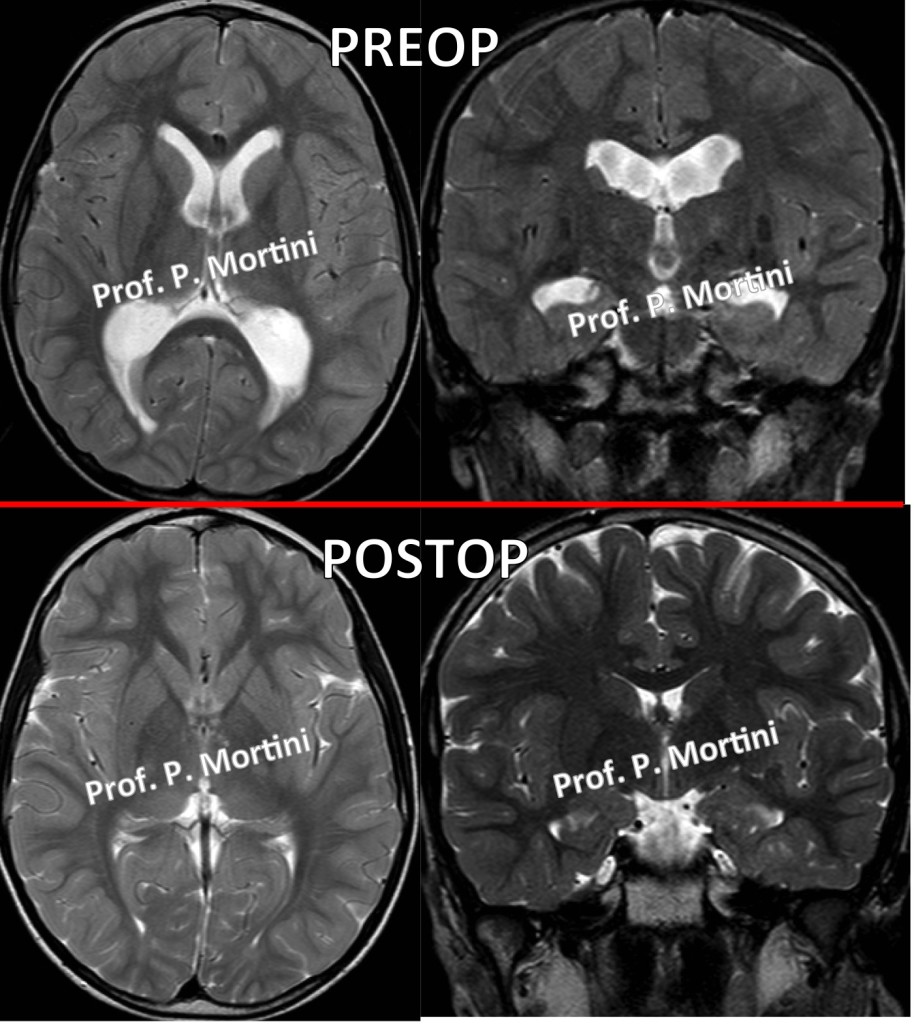
The adult brain usually produces about one half liter (500cc) of Cerebro Spinal Fluid – CSF daily in spaces within the brain called ventricles.
The CSF circulates out of the ventricles, bathes the brain and spinal cord, and is reabsorbed into the bloodstream.
Hydrocephalus usually results either from:
- an imbalance between CSF production and absorption (communicating hydrocephalus); or
- when there is a blockage within the ventricular system such as a tumor that prevents CSF circulation (obstructive hydrocephalus).
Adult communicating hydrocephalus is most commonly referred to as Normal Pressure Hydrocephalus (NPH). However this is a misnomer, as the pressure may or may not be normal in a given patient.
NPH usually occurs in older adults, with the majority of affected patients over 60 years of age. Most cases of adult communicating hydrocephalus/NPH are primary/idiopathic and of unknown cause.
Some patients develop secondary NPH in association with or following subarachnoid hemorrhage, head injury, brain tumor, or meningitis.
Depending on the cause and type of hydrocephalus, a variety of neurosurgical interventions may be used for treatment.
Adult Communicating Hydrocephalus/Normal Pressure Hydrocephalus (NPH)
Symptoms
NPH has three primary symptoms:
- gait disturbance/imbalance
- urinary frequency/incontinence
- cognitive slowing/short term memory difficulty/dementia
Diagnosis
Each of the primary symptoms has many other causes in the elderly population, and no combination of the cardinal symptoms is absolutely diagnostic.
The symptoms often develop slowly over a long period of time, and are mistaken for “normal aging”.
The ventricles enlarge with normal aging and with degenerative diseases such as Alzheimer’s disease.
All described diagnostic tests have false positives and negatives. No test is perfect in its ability to diagnose this condition.
Patient evaluation
1) Patients are evaluated by our multidisciplinary, experienced team composed of Movement Disorder Neurology, Cognitive/Aging Neurology, Neuroradiology, and Neurosurgery.
2) Patients undergo an MRI (CT scanning if pacemaker present).
3) Spinal fluid drainage to determine to what degree they improve with a test removal of spinal fluid.
A small catheter is placed into the lumbar (lower back) spinal fluid space, allowing spinal fluid removal over 2-3 days.
Treatment
Ventricular shunt surgery: If a patient’s symptoms improve with spinal fluid drainage, a shunt surgery is proposed. The goal of a shunt is to divert CSF into another region of the body where it can be absorbed.
The shunt is a soft tube that is implanted either within the skull or under the skin. Between the shunt catheter in the brain and the catheter that goes to the abdomen or bloodstream, there is a one way valve that regulates CSF flow through the shunt. If there is too much flow, the ventricles will collapse and bleeding can occur. If there is too little flow, the patient’s symptoms will not improve.
A valve inside the shunt allows us to fine tune the shunt function over time. The shunt is implanted under general anesthesia
Longitudinal Follow-up
Long term follow up of shunt function is necessary to minimize complications and maximize benefits. Shunt valves often need to be reprogrammed over time to get the best clinical benefit in a given patient.
 English
English Italiano
Italiano