Clinically nonfunctioning pituitary adenomas make up about half of pituitary adenomas. The vast majority of them are benign.
There are several possible reasons why nonfunctioning pituitary adenomas could occur:
- Typically, the body produces hormones by taking a larger molecule and cutting it at the right places to create a functioning hormone. In some cases, something is wrong with this cutting process and a “functional” hormone is not made. The hormone might still travel into the bloodstream, but it is inactive and usually cannot be detected using standard blood tests.
- In some cases, the hormone might be formed inside the cell, but there is something wrong with the transport process that is required to release it into the blood stream.
- In other cases, the tumor cells simply do not produce a hormone
Symptoms
The most common symptoms are due to the large tumor compressing nearby structures, leading to:
- Vision loss
o When large pituitary adenomas (macroadenomas) grow upward into the brain cavity, the tumor can elevate and compress the optic chiasm.
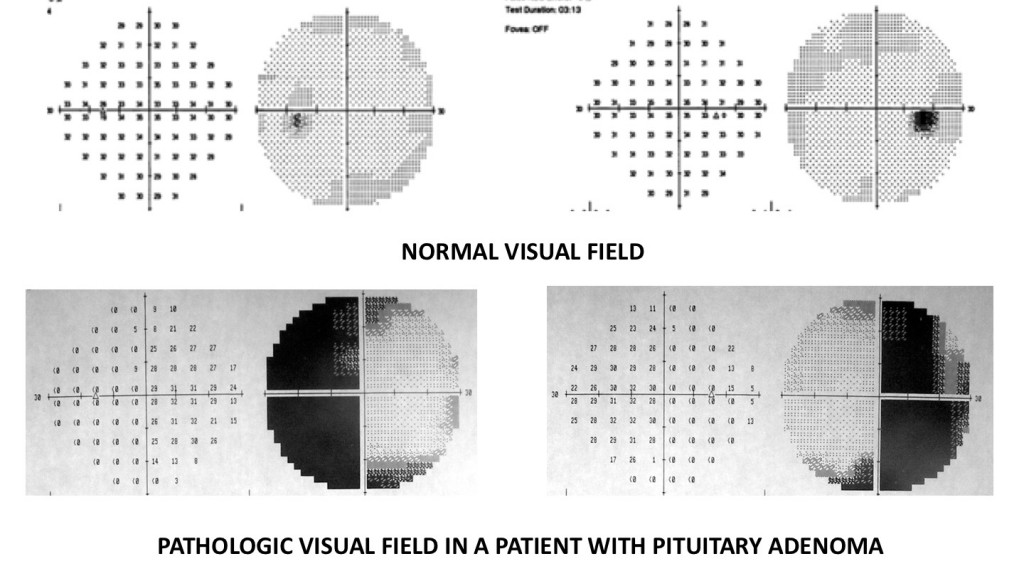
o A loss of the outer peripheral vision, called a bitemporal hemianopsia
When severe, a patient can only see what is directly in front of them; many patients do not become aware of their visual loss until it is quite severe.
- Other visual problems include:
o Loss of visual acuity (blurry vision), especially if the macroadenoma grows forward and compresses an optic nerve
o Inability to perceive colors as brightly as usual
Diagnosis
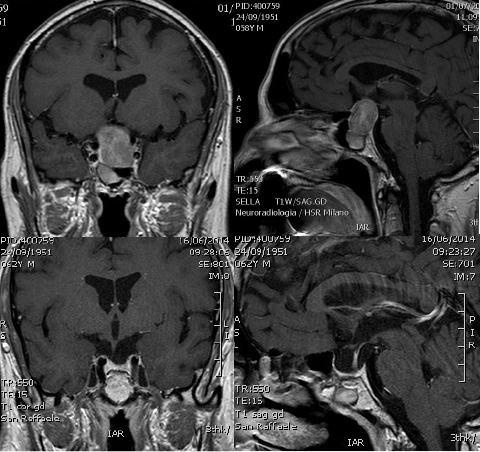
Imaging scans are one method doctors use to diagnose clinically nonfunctioning pituitary adenomas.
Hormone tests are also indicated to evaluate the levels of pituitary hormone, confirming that there is no evidence of hormone production by the tumor.
Necessary investigations may be:
- Magnetic resonance imaging (MRI) scan
- Hormone test
- Vision test
If your symptoms suggest pituitary failure (hypopituitarism), a complete evaluation of the endocrine system may be advisable. Based on results of these blood tests, you may undergo additional hormonal studies.
If you are experiencing vision problems, an experienced ophthalmologist can evaluate you. The evaluation should include:
- Acuity testing of each eye
- Formal visual field testing
This will determine if you have a loss of peripheral vision.
Treatment option
- Surgery
- Radiation Therapy
Surgery for Clinically Nonfunctioning Pituitary Adenomas
For most patients with nonfunctional adenomas, surgically removing the adenoma is the most effective treatment.
The extent of surgical removal, which is related to:
- Tumor size
- If the tumor invaded the cavernous sinus (the compartments on either side of the pituitary sella)
- If the tumor expanded into the brain cavity
- If the surgeon was able to remove the entire tumor, the cure rate is 70 percent to 80 percent.
Overall, surgery improves:
- Vision in 75 to 90 percent of patients
- Headache in 80 to 90 percent of patients
- Suppressed pituitary function in 10 to 30 percent of patients
If the pituitary adenomas require surgery, typically the best procedure is through a nasal approach.
The minimally invasive endoscopic endonasal technique
This procedure removes the tumor while minimizing complications, hospital time and discomfort. This advanced technique requires specialized training and equipment.
Very large tumors that extend into the brain cavity may require opening the skull (craniotomy) to access the tumor.
If, after your surgery, some tumor cells remained or regrew, you may be a candidate for radiation therapy or a repeat surgery.
Radiation Therapy
Radiation therapy as a second-line therapy for endocrine-inactive tumors. Focused-beam radiation, named Stereotactic Radiosurgery can be effective in controlling tumor growth. In some cases, radiation therapy may cause a loss of pituitary function.
Acromegaly Cushing Disease Prolactinomas TSH-oma
 English
English Italiano
Italiano