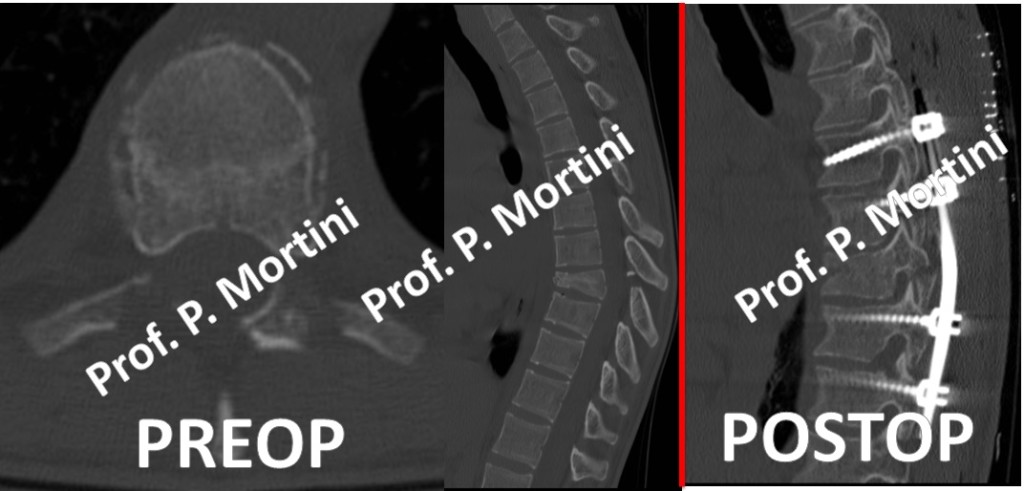
Spinal trauma is caused by damage to the spinal cord that results in
- a bruise (also called a contusion)
- a partial tear
- a complete tear
Because the spinal cord is the central carrier of signals throughout the body, damage to the spinal cord can have serious consequences.
A spinal cord injury, depending on its location and severity, may result in a partial or total loss of movement, sensation, and organ function.
There is a range of severity in spinal cord injuries. A mild contusion of the spinal cord may cause the loss of only some function below the site of the injury.
A complete transection, or severing of the spinal cord, is a total and permanent loss of sensation and movement below the site of the transection.
Patients with spinal trauma also are likely to develop infections of the bladder, lungs, and skin.
Causes
The primary causes of spinal cord injury are motor vehicle accidents, violence, falls and sports.
Symptoms
The initial symptom of spinal cord injury often is spinal shock, which can cause a loss of feeling and movement below the site of the injury.
Lasting from a few hours to a few weeks, spinal shock may subside over time to reveal the true extent of the injury. Other immediate symptoms may include
- muscle spasticity
- difficulty breathing
- heart rate and blood pressure problems
- loss of bladder and bowel function
Long-term effects of spinal trauma vary depending on the location and severity of the injury. The body below the site of the injury is affected, so the higher the injury occurs in the spinal column, the more severe the symptoms usually are.
For example, an injury in the cervical spine will affect all of the limbs, as well as the muscles that control breathing and other essential functions. An injury in the lumbar spine, however, will affect the lower extremities and bowel and bladder function, but usually will not damage other organs or systems.
Complete injuries high in the neck and trauma complicated by other serious injuries may result in death or require total care for the rest of the patient’s life.
Diagnosis
Diagnosis and management of spinal trauma can be difficult and a missed injury can cause serious complications. In the cases of accidents in which a spinal injury is suspected, it must be assumed until proven otherwise.
The spine must be protected and immobilized at all times during assessment and diagnosis. Initial assessment includes a clinical exam and also may include imaging tests, including x-rays, computed tomography (CT) scans, and magnetic resonance imaging (MRI) scans.
The tests should include the entire spine, not just the region where the injury is suspected. The choice of diagnostic techniques varies based on the state of the patient consciousness and the presence of other injuries.
The condition of a patient immediately after a spinal trauma may not necessarily indicate the long-term effects of the injury, so an ongoing series of comprehensive medical evaluations and imaging tests are necessary to understand the extent of the injury.
Treatment
Spinal trauma requires immediate treatment, usually at the site of the injury, to prevent additional injury to the spinal cord. Initial intervention includes immobilization of the head, neck, and back, and steroid medications to control swelling.
Sometimes immediate surgery is necessary to evaluate the state of the spinal cord, stabilize fractured vertebrae, release pressure from the injured area, and treat injuries to other parts of the body.
There is no way to regenerate nerve tissue that has been damaged, but ongoing treatment may allow some people with spinal trauma to regain some feeling and function. Physical, occupational, and speech therapy and rehabilitation are important parts of the long-term recovery process.
Depending on the severity of the injury, long-term intervention may be necessary to maintain everyday function. This may include mechanical ventilation to assist in breathing, a catheter to drain the bladder, or a feeding tube to provide extra nutrition and calories.
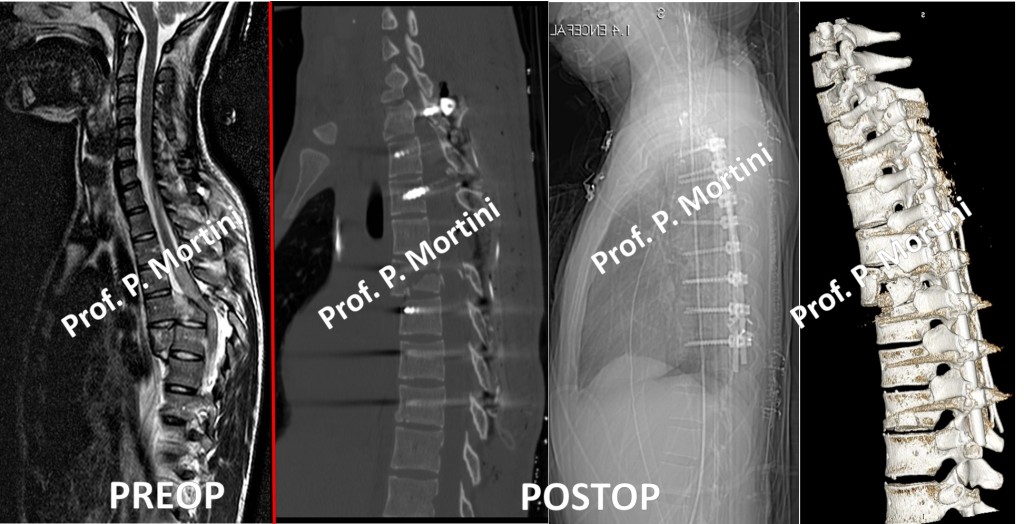
 English
English Italiano
Italiano