The spinal cord is surrounded by a protective membrane called the meninges, which is made up of three layers
- the dura mater
- the arachnoid membrane
- the pia mater
Tumors that arise from this tissue, especially the cells that make up the arachnoid membrane (arachnoid cap cells), are called meningiomas.
Meningiomas usually are benign, slow-growing tumors, although in rare cases they may be malignant and invade surrounding tissue.
Meningiomas account for approximately 25% of spinal canal lesions. They can occur at any location throughout the spine, but predominate in the thoracic region (probably because this is the largest segment).
Spinal Meningiomas occur approximately four times as often in women as in men, and the average age is 45 years.
Symptoms
The symptoms of a meningioma are caused by the pressure the growing tumor exerts on surrounding tissue. These tumors can occur in a variety of places and therefore cause a wide range of symptoms.
Depending on the location of the mass, meningiomas may cause
- headaches
- nausea
- seizures
- weakness or numbness in the limbs or face
- visual problems
- gradual changes in mood or personality.
The symptoms tend to increase in severity as the tumor grows in size.
Diagnosis
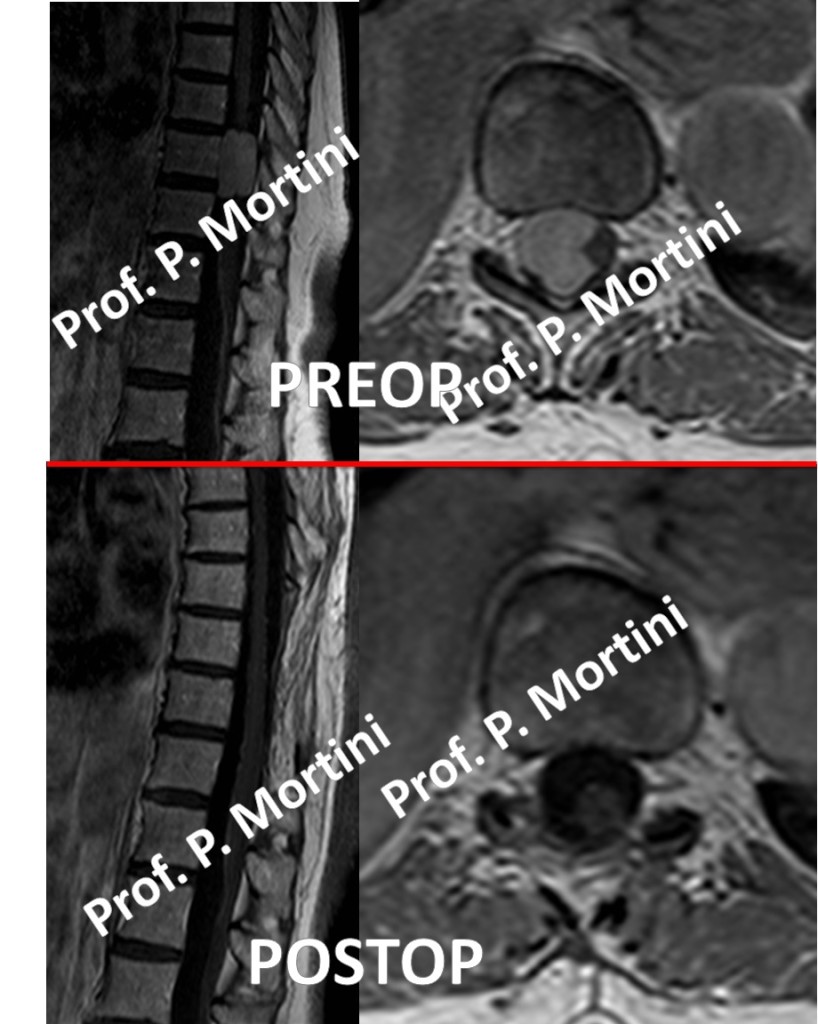
Imaging studies are the key component in the diagnosis of meningiomas. Computed Tomography (CT) and Magnetic Resonance Imaging (MRI) scans are used to provide detail about the tumors size, location, and effect on surrounding structures. In addition, an angiogram, which allows physicians to visualize the blood vessels in the area, may be used.
Treatment
If a meningioma is small and does not cause symptoms, it may be observed over time rather than treated immediately.
In cases in which treatment is necessary, the first line of treatment for these tumors usually is surgery. Because the tumors are benign, complete resection often results in a cure.
Some tumors, however, may be difficult to remove completely. In addition, meningiomas may recur even in cases of complete resection. When a tumor is removed, it can be examined under a microscope to assess the risk of recurrence and dictate the next step in treatment.
Radiation therapy may be used as a follow-up treatment, especially for malignant tumors but it is not recommended for children under the age of two.
In addition, stereotactic radiosurgery, which involves the use of a highly focused beam of radiation to target the tumor, may be used as either primary or adjunct treatment.
Chemotherapy has yet to show benefits for children with meningiomas, although treatments that affect hormonal processes are being investigated because these tumors are believed to have some hormonal involvement.
 English
English Italiano
Italiano